Pacslens puts AI between your PACS worklist and the radiologist — so a suspected intracranial hemorrhage at 3 a.m. never waits behind a routine knee MRI.
Flags suspected ICH, PTX, and PE within 90 seconds of DICOM acquisition.
The model is trained on 1.4 million de-identified chest and head CT studies annotated by board-certified radiologists, achieving 96.2% sensitivity on held-out community hospital data for three primary critical-finding categories — intracranial hemorrhage, pneumothorax, and pulmonary embolism. Flagged studies jump to the top of the active worklist and trigger an HL7 ORU notification to the ordering provider immediately, regardless of how many other studies are queued.
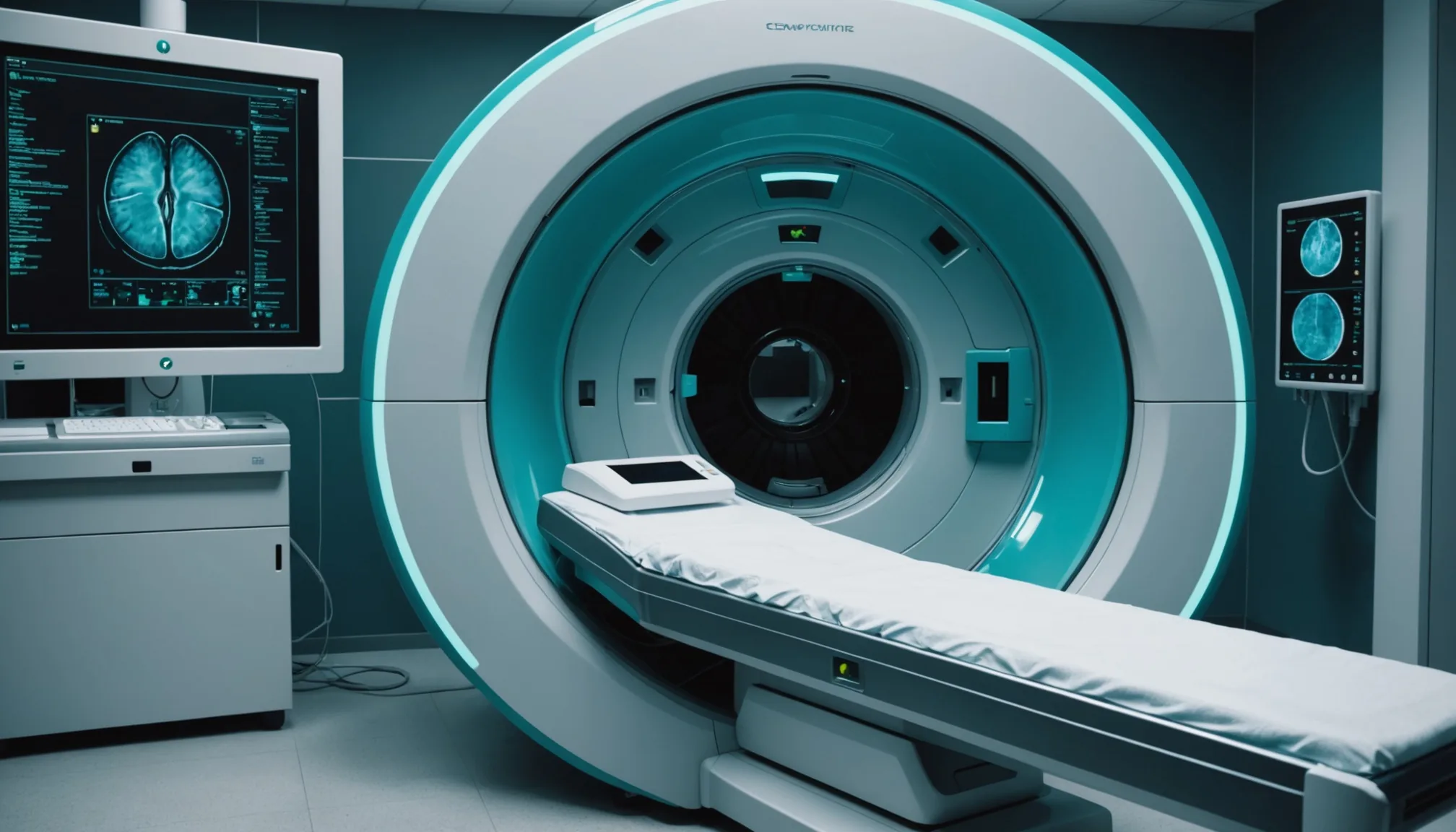
AI-generated preliminary structured findings narrative before the radiologist opens the study.
For every chest, head, and abdominal CT, Pacslens generates a structured pre-read note that identifies abnormal organ systems, retrieves relevant priors from the PACS archive, and surfaces incidental findings that need follow-up language. The note appears as a collapsible panel inside the radiologist’s existing viewer. Accepted elements pre-populate the structured reporting template, cutting average report-generation time by an estimated 6–9 minutes per study.
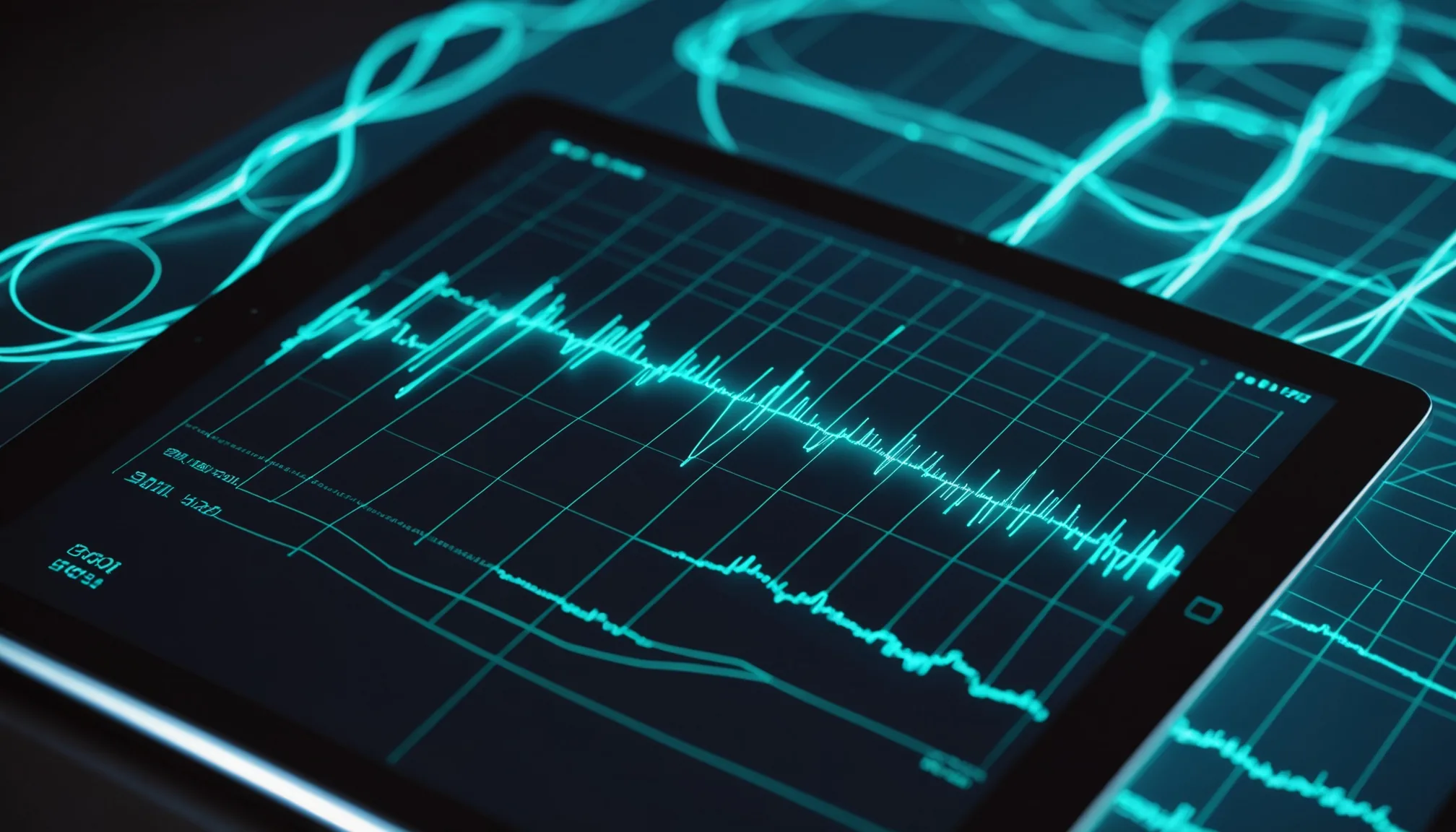
Dynamic worklist re-ordering by predicted urgency, study age, and patient acuity score.
Pacslens re-orders the active worklist continuously using a composite urgency score built from AI triage classification, study age, ordering provider priority, and patient acuity from the ADT feed. Studies approaching the department’s target turnaround time are promoted before they breach. The result is a read sequence a single radiologist can follow end-to-end — no manual queue sorting needed during high-volume overnight coverage.

Pacslens connects to your existing PACS via HL7 feed after a one-time IT configuration. No manual routing. No secondary viewer login. No change to the radiologist’s reading environment.
DICOM studies are transmitted from the hospital PACS worklist in real time as each scan completes on the modality. Pacslens receives the study via HL7 feed — no manual routing or IT intervention needed after initial configuration with Epic Radiant, Cerner RadNet, or MEDITECH Expanse Imaging.
A fast-triage model classifies each study by urgency within 90 seconds of DICOM receipt. The model flags suspected intracranial hemorrhage, pneumothorax, and pulmonary embolism findings using thresholds calibrated on community hospital CT volumes, not academic medical center case mix.
Flagged and time-sensitive studies are re-sorted to the top of the radiologist’s active PACS worklist. A second model generates a structured pre-read summary with relevant prior studies from the archive, delivered as a collapsible panel in the existing viewer without requiring a separate application.
Critical-finding alerts are pushed via HL7 ORU R01 message (or FHIR Task for FHIR-enabled EHRs) to the ordering provider’s in-basket in Epic or Cerner within 60 seconds of triage classification. Every alert is timestamped and logged for ACR Critical Results Communication compliance reporting.
Every inbound DICOM study is classified by urgency within 90 seconds of acquisition on the modality — fast enough to surface a critical finding before the ordering provider has left the scanner room.
96.2% sensitivity on held-out community hospital data for the three primary critical-finding categories: intracranial hemorrhage, pneumothorax, and pulmonary embolism. Trained on 1.4 million annotated chest and head CT studies.
Structured pre-read summaries that pre-populate the reporting template reduce average report-generation time by an estimated 6–9 minutes per study — time that compounds across 180–400 studies a day.
We work with community hospitals and regional health systems running Sectra, Agfa, Epic Radiant, and Cerner RadNet. If you handle 150–600 imaging studies per day with a team of 2–8 radiologists, we built this for you.